Macros for Diabetes (Type 2): A Complete Nutrition Guide
Reviewed by Sarah Chen, MS, RD

Managing type 2 diabetes can feel like a constant balancing act. You’re trying to control your blood sugar, manage your weight, reduce medication, and prevent long-term complications. The nutritional advice you get is often vague: “eat healthy,” “watch your carbs,” “use the plate method.”
While these are good starting points, they lack the precision needed for optimal blood sugar control. If you want to take your diabetes management to the next level, understanding and tracking macronutrients is the most powerful tool you have. New to tracking? Start with our beginner’s guide to counting macros.
By controlling your intake of protein, fat, and especially carbohydrates, you can directly influence your blood sugar levels, improve your body’s sensitivity to insulin, and potentially reduce your reliance on medication.
This guide provides a comprehensive, evidence-based approach to setting your macros for type 2 diabetes. We’ll cover everything from carb counting and protein needs to the role of healthy fats and how to use a glucose monitor to fine-tune your diet.
CRITICAL MEDICAL DISCLAIMER: This guide is for informational purposes only. You MUST work with your endocrinologist or healthcare provider before making any significant dietary changes. Changing your macro intake, especially carbohydrate intake, will likely require adjustments to your medication (like insulin or sulfonylureas) to prevent dangerous hypoglycemia (low blood sugar).
For a guide on the precursor to Type 2 Diabetes, see our article on macros for insulin resistance.

Type 2 Diabetes and Macronutrients
In type 2 diabetes, your body has become resistant to insulin, the hormone that helps shuttle glucose (sugar) from your blood into your cells. This means that after you eat, especially carbohydrates, your blood sugar can rise to dangerously high levels.
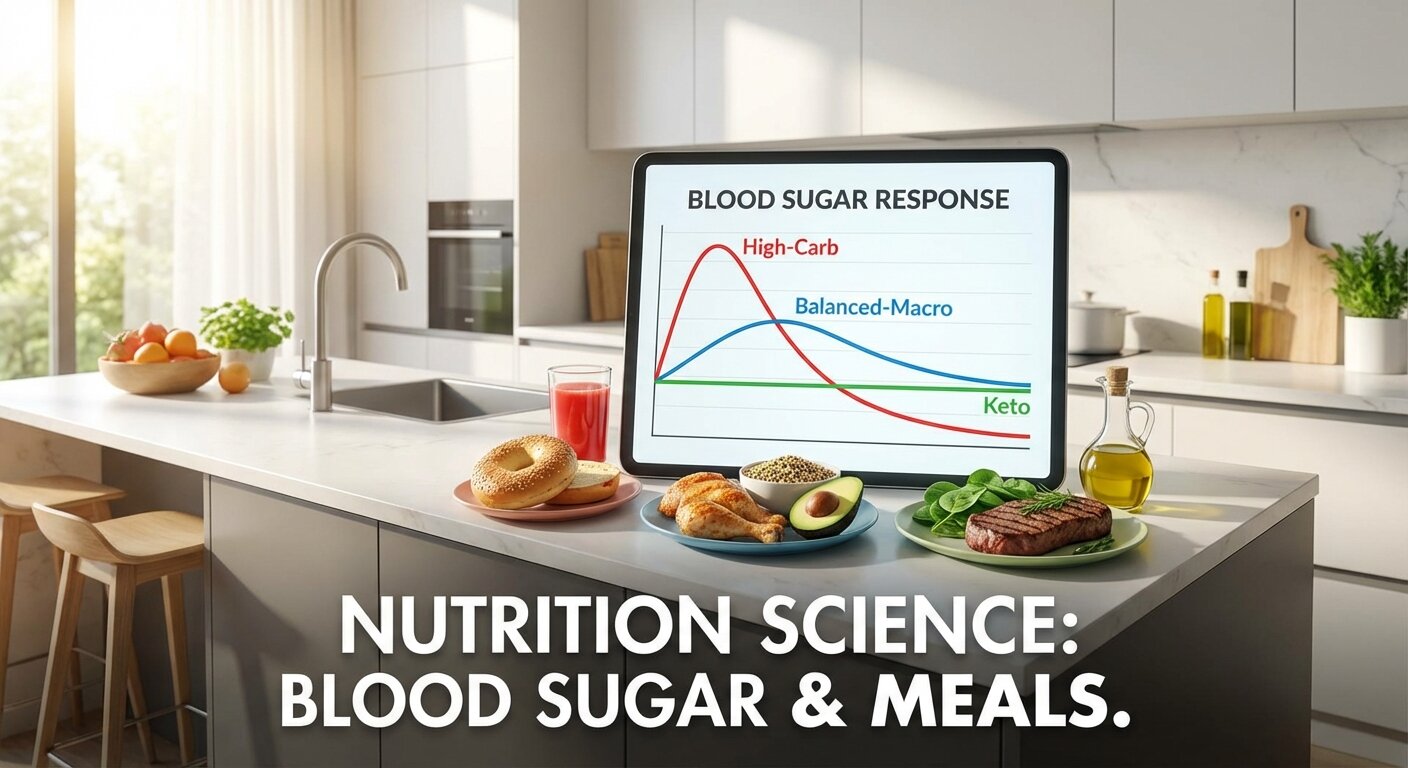
Each macronutrient affects your blood sugar differently:
- Carbohydrates: Have the largest and fastest impact. They break down directly into glucose, causing a significant rise in blood sugar.
- Protein: Has a minimal impact. It can be converted to glucose in a slow, demand-driven process, but it doesn’t cause a sharp spike.
- Fat: Has virtually no direct impact on blood sugar. It slows down the digestion of carbs, which can actually help blunt the blood sugar response.
Therefore, the cornerstone of diabetes management is controlling carbohydrate intake and balancing it with adequate protein and healthy fats.
Recommended Macro Ratios for Type 2 Diabetes
While the American Diabetes Association (ADA) has historically promoted a higher-carb diet, modern research strongly supports a lower-carb, higher-protein approach for better glycemic control.
The Optimal Starting Point
40% protein / 30% carbs / 30% fat
Why this ratio works for diabetics:
- High Protein: Minimizes blood sugar spikes, promotes satiety for weight management, and helps maintain muscle mass, which is crucial for insulin sensitivity.
- Moderate Carbs: Provides enough energy while significantly reducing the glucose load on your system, leading to lower A1C and less need for medication.
- Moderate Fat: Promotes satiety and slows down carb absorption, helping to stabilize blood sugar.
In grams (for a 2,000-calorie diet):
- Protein: 200g
- Carbs: 150g
- Fat: 67g
This ratio is a powerful starting point for most people with type 2 diabetes.
Alternative Ratios
Not everyone’s needs are the same. Your ideal macro split can depend on your medication, activity level, and personal tolerance to carbohydrates.
| Approach | Protein % | Carb % | Fat % | Best For |
|---|---|---|---|---|
| Moderate Carb | 40% | 30% | 30% | Most people with T2D, sustainable long-term. |
| Lower Carb | 35% | 25% | 40% | Those needing tighter control, less active individuals. |
| Very Low Carb (Keto) | 25% | 5-10% | 65-70% | People aiming for diabetes remission, requires strict medical supervision. |
The key takeaway: Protein should be high, and carbohydrates should be controlled. The exact percentage can be tailored to your body’s response.
Carbohydrates for Diabetics: Quality and Quantity
For diabetics, managing carbs is the number one priority.
How Many Carbs Should You Eat?
- Moderate Carb (Recommended Start): 100-150g per day. This is a significant reduction from the standard diet and usually yields excellent results.
- Lower Carb: 50-100g per day. Can provide even tighter blood sugar control.
- Keto: Under 50g per day. Most aggressive approach, requires doctor supervision.
Important: Reducing your carb intake will lower your blood sugar. If you take insulin or sulfonylureas (like glyburide, glipizide), your dosage must be adjusted by your doctor to avoid life-threatening hypoglycemia.
Carb Quality is Critical
The type of carbohydrate you eat is just as important as the amount. Focus on low-glycemic, high-fiber sources.
Best Carb Sources:
- Non-Starchy Vegetables: Broccoli, cauliflower, spinach, kale, bell peppers, zucchini (eat abundantly).
- Legumes: Lentils, chickpeas, black beans.
- Low-Sugar Fruits: Berries, apples, pears.
- Whole Grains (in strict moderation): Quinoa, steel-cut oats, barley.
Carbs to Avoid:
- Sugary Foods: Soda, juice, candy, desserts.
- Refined Grains: White bread, white rice, pasta, cereal.
- Starchy Vegetables: White potatoes, corn.
- Most Processed Foods: They often contain hidden sugars and refined carbs.
Carb Counting and Timing
- Carb Counting: Track your carb intake diligently using an app like MyFitnessPal or Cronometer. This is essential for understanding how your diet affects your blood sugar.
- Pairing: Never eat a “naked carb.” Always pair carbohydrates with a source of protein and/or fat to slow down digestion and prevent a sharp blood sugar spike.
- Timing: Spread your carbohydrate intake throughout the day rather than consuming it all in one large meal.
Protein for Blood Sugar Control
Protein is a diabetic’s best friend.
Why Prioritize Protein?
- Minimal Blood Sugar Impact: Protein does not cause a significant rise in blood sugar.
- High Satiety: It keeps you full, making it easier to manage weight and avoid snacking on carbs.
- Preserves Muscle: Maintaining muscle mass is crucial for improving insulin sensitivity.
How Much Protein?
Target: 1.0-1.2g per pound of your ideal body weight.
This is higher than the RDA, but research shows it is safe and beneficial for diabetics, provided you do not have advanced kidney disease.
Example (Goal weight of 175 lbs):
- 175g - 210g of protein per day.
Kidney Health Note: If you have been diagnosed with chronic kidney disease (CKD), consult your nephrologist about your protein intake. For most diabetics without advanced CKD, a high-protein diet is considered safe.
Best Protein Sources
- Lean meats (chicken, turkey)
- Fatty fish (salmon, mackerel for omega-3s)
- Eggs
- Greek yogurt (plain, unsweetened)
- Cottage cheese
- Tofu and edamame
- Quality protein powders
Healthy Fats for Diabetics
Fat has no direct impact on blood sugar and plays a supportive role in a diabetic diet.
Why Include Healthy Fats?
- Slows Digestion: Helps to blunt the blood sugar response from meals containing carbohydrates.
- Satiety: Keeps you feeling full and satisfied.
- Heart Health: Diabetics are at higher risk for heart disease. Monounsaturated and omega-3 fats are cardioprotective.
Best Fat Sources
- Monounsaturated Fats: Avocado, olive oil, almonds, macadamia nuts.
- Omega-3 Fats: Salmon, sardines, walnuts, flaxseeds, chia seeds.
Fats to Limit
- Saturated Fats: From processed meats and high-fat dairy.
- Industrial Seed Oils: Soybean, corn, sunflower oils.
- Trans Fats: Avoid completely.
Tracking Macros and Blood Sugar: The Feedback Loop
The key to mastering your diabetes is understanding your personal response to food.
Using a Glucose Monitor
Your glucometer or Continuous Glucose Monitor (CGM) is your most valuable tool.
- Continuous Glucose Monitor (CGM): The gold standard. It allows you to see your blood sugar trends 24/7 and directly observe how specific meals affect you. If your insurance covers a CGM, it’s a game-changer.
- Standard Glucometer: If you don’t have a CGM, test strategically:
- Before a meal (your baseline).
- 1 hour after the first bite (the peak).
- 2 hours after the first bite (how well you’ve returned to baseline).
Your goals (general guidelines, consult your doctor):
- Fasting: < 130 mg/dL (ideally < 100 mg/dL)
- 2 hours post-meal: < 180 mg/dL (ideally < 140 mg/dL)
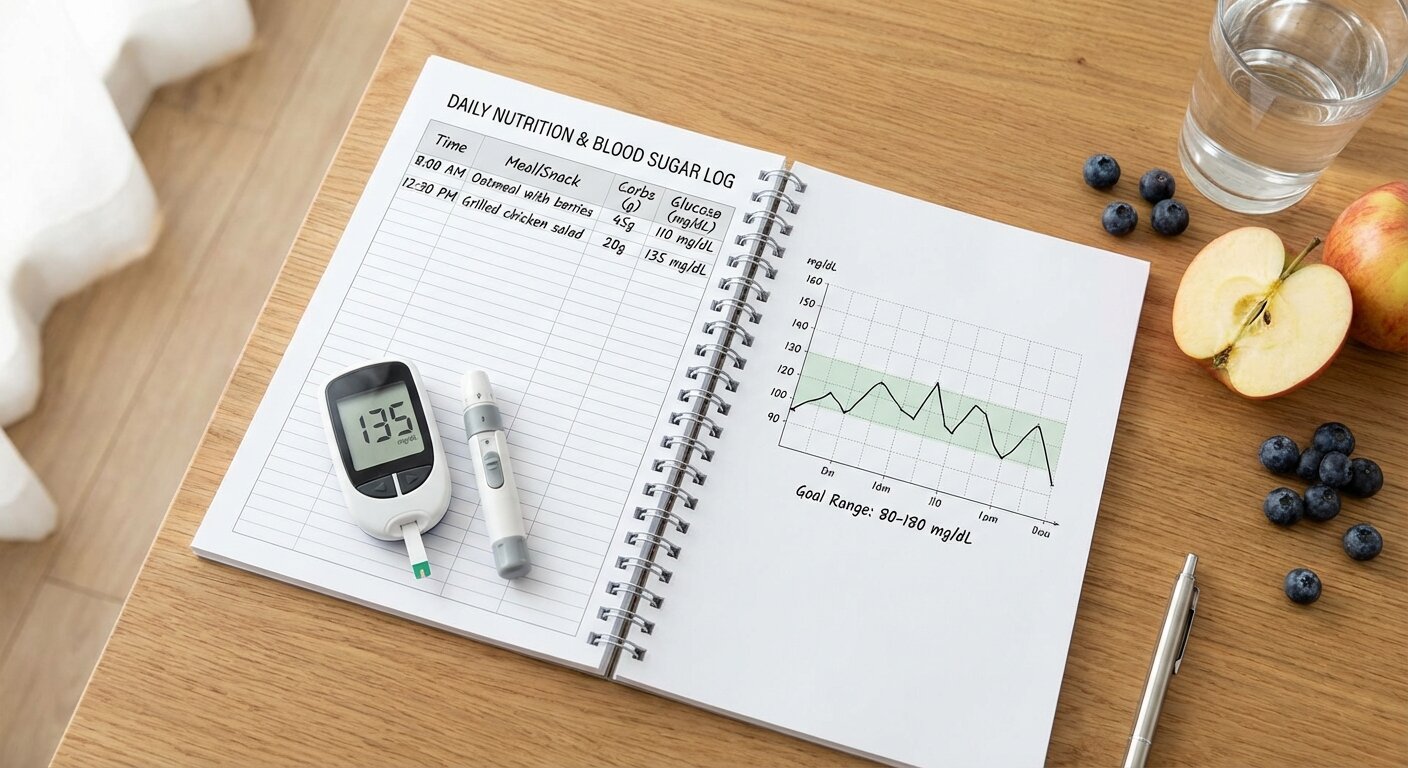
The Process
- Plan a meal with specific macros (e.g., 40g protein, 30g carbs, 20g fat).
- Measure and track the food accurately.
- Test your blood sugar before, 1 hour after, and 2 hours after.
- Analyze the result. Did you stay in range? If not, the meal may have had too many carbs for you, or the wrong type of carbs.
- Adjust and repeat. Use this feedback to fine-tune your personal macro and food choices.
Weight Loss and Type 2 Diabetes Remission
For many, type 2 diabetes is driven by excess body fat, particularly visceral fat around the organs. Losing this weight is the most effective way to improve insulin sensitivity and potentially put diabetes into remission.
Remission: This means your blood sugar levels return to the non-diabetic range without needing medication. It’s not a “cure,” as the condition can return if weight is regained, but it is a realistic and life-changing goal for many.
The Strategy
- Create a Calorie Deficit: Use your calculated macros within a 300-500 calorie deficit.
- Prioritize Protein: Maintain high protein intake (1.2g/lb) to ensure you are losing fat, not muscle.
- Strength Train: Build muscle to improve your body’s ability to handle glucose.
- Be Consistent: Remission is the result of sustained lifestyle changes over months, not weeks.
Sample Diabetic Meal Plan
Target: 1,800 calories | 180g protein (40%) | 135g carbs (30%) | 60g fat (30%)
Breakfast
- Greek Yogurt Bowl: 1.5 cups plain Greek yogurt, 1/2 cup berries, 1/4 cup walnuts.
- Macros: ~40g protein, 30g carbs, 20g fat
Lunch
- Large Grilled Chicken Salad: 8 oz grilled chicken breast on a bed of spinach with non-starchy veggies and an olive oil-based dressing.
- Macros: ~60g protein, 15g carbs, 15g fat
Snack
- Protein Shake: 1 scoop of whey or casein protein powder mixed with water or unsweetened almond milk.
- Macros: ~25g protein, 5g carbs, 2g fat
Dinner
- Baked Salmon with Asparagus and Quinoa: 8 oz salmon fillet, a large serving of roasted asparagus, and 1/2 cup of cooked quinoa.
- Macros: ~55g protein, 30g carbs, 20g fat
Note: This plan is an example. Your specific portions and food choices should be tailored to your calorie and macro targets, and your individual blood sugar responses.
A Note on Type 1 vs. Type 2 Diabetes
This guide is focused on Type 2 Diabetes, which is characterized by insulin resistance.
Type 1 Diabetes is an autoimmune condition where the body does not produce insulin. While carb counting is also essential for Type 1 management, it is for the purpose of matching insulin doses, not necessarily for restriction. Type 1 diabetics must work with their endocrinologist to manage their insulin-to-carb ratios.
FAQ: Diabetes and Macros
What are the best macros for a type 2 diabetic?
For type 2 diabetes, a macro ratio of 40% protein, 30% carbs, and 30% fat is an excellent starting point. This high-protein, moderate-carb, and moderate-fat approach helps control blood sugar, improve insulin sensitivity, and promote satiety, often leading to better A1C levels and reduced medication needs.
How many carbs should a type 2 diabetic eat per day?
Most people with type 2 diabetes see significant blood sugar improvement with 100-150g of carbohydrates per day. Those on lower-carb plans may go down to 50-100g. It’s crucial to focus on high-fiber, low-glycemic carbs and to work with your doctor, as medication may need adjustment.
Can you reverse type 2 diabetes with diet?
Type 2 diabetes can often be put into remission, meaning blood sugar levels return to a non-diabetic range without medication. This is typically achieved through significant lifestyle changes, including a macro-controlled diet, weight loss, and regular exercise. It’s not a cure, as symptoms can return if lifestyle changes are not maintained.
Is keto safe for diabetics?
A ketogenic diet can be very effective for managing type 2 diabetes, but it must be done under strict medical supervision. Because it drastically lowers carbohydrate intake, medications like insulin or sulfonylureas must be adjusted to prevent dangerous hypoglycemia (low blood sugar).
How much protein should a diabetic eat?
Aim for 1.0-1.2g of protein per pound of ideal body weight. High protein intake is beneficial for diabetics as it has minimal impact on blood sugar, increases satiety to help with weight management, and preserves muscle mass, which is vital for insulin sensitivity.
Do I need to count macros if I have diabetes?
While not strictly necessary for everyone, counting macros provides a much higher level of precision and control over blood sugar than other methods like the plate method. It helps you understand exactly how your body responds to different amounts of protein, fat, and carbs, leading to better management.
What is the best way to track my blood sugar response to food?
Using a Continuous Glucose Monitor (CGM) is the best way to see your blood sugar response in real-time. If you use a standard glucometer, test before your meal and then 1-hour and 2-hours after to see how a specific food impacts you. Aim for post-meal readings below 180 mg/dL, ideally below 140 mg/dL.
What is the difference between type 1 and type 2 diabetes?
Type 1 diabetes is an autoimmune disease where the body attacks and destroys insulin-producing cells; it requires insulin therapy. Type 2 diabetes, which this guide focuses on, is a condition of insulin resistance where the body doesn’t use insulin effectively. It is primarily managed with lifestyle changes and oral medications, though insulin may be needed in later stages.
Related Resources
Disclaimer: This content is for informational purposes only. Consult a healthcare provider before making changes to your diet.


