Macros for Insulin Resistance: A Complete Nutrition Guide
Reviewed by Sarah Chen, MS, RD

You feel tired all the time, especially after meals. You crave carbs and sugar constantly. You’re gaining weight, particularly around your belly, and it feels impossible to lose.
If this sounds familiar, you might be dealing with insulin resistance.
Insulin resistance affects an estimated 1 in 3 adults and is a precursor to pre-diabetes and type 2 diabetes. It’s a metabolic condition where your body’s cells stop responding properly to the hormone insulin, leading to a cascade of issues from weight gain to hormonal disruption.
The good news? Insulin resistance is not a life sentence. It can be significantly improved—and often reversed—with the right nutrition and lifestyle changes. And the single most powerful tool you have is managing your macronutrients.
This guide explains what insulin resistance is, how macros affect it, and how to set up your diet to improve your insulin sensitivity, stabilize your energy, and take back control of your metabolic health.
Medical Disclaimer: This guide is for informational purposes. Always work with a healthcare professional to diagnose and manage insulin resistance, especially if you are on medication for diabetes or blood pressure.
New to macronutrients? Start with our complete guide to macronutrients to understand protein, carbs, and fats. Then use our Macro Calculator and select a lower-carb, higher-protein split for insulin resistance management.

Understanding Insulin Resistance
Before we talk macros, let’s understand the problem.
What Is Insulin?
Insulin is a hormone made by your pancreas. Its main job is to help your cells absorb glucose (sugar) from your bloodstream for energy.
Think of insulin as a key:
- It unlocks your cells (muscle, fat, liver)
- It allows glucose to enter and be used for fuel
What Is Insulin Resistance?
Insulin resistance is when your cells stop responding to insulin’s signal. The “lock” on your cells becomes rusty and the insulin “key” no longer works properly.
What happens next:
- Glucose can’t enter cells easily, so it builds up in your blood.
- Your pancreas senses high blood sugar and pumps out even more insulin to try to force the cells to respond.
- This leads to chronically high levels of both blood sugar and insulin (hyperinsulinemia).
Why Is High Insulin a Problem?
High insulin levels are the root cause of many metabolic issues:
- Fat storage: Insulin is a fat-storage hormone. High levels tell your body to store fat, especially in the abdominal area.
- Blocks fat burning: High insulin prevents your body from accessing and burning stored fat.
- Increased hunger and cravings: Blood sugar rollercoasters lead to intense cravings for carbs and sugar.
- Inflammation: High insulin is pro-inflammatory.
- Hormonal disruption: In women, it can lead to PCOS. In men, it can lower testosterone.
- Progression to diabetes: Eventually, the pancreas can’t keep up, and blood sugar rises to diabetic levels.
Symptoms of Insulin Resistance
- Fatigue, especially after meals (“food coma”)
- Intense cravings for sugar or carbohydrates
- Difficulty losing weight, especially belly fat
- Darkened skin patches (acanthosis nigricans) on the neck or armpits
- Skin tags
- High blood pressure
- High triglycerides
- For women: PCOS symptoms like irregular periods
You can have insulin resistance for years without knowing it, as your body compensates by producing more insulin. A fasting insulin blood test is the best way to diagnose it.
Best Macro Ratios for Insulin Resistance
Managing insulin resistance is all about controlling insulin levels. Since carbohydrates have the biggest impact on insulin, a lower-carb, higher-protein approach is most effective.
Recommended Starting Point
35-40% protein / 25-35% carbs / 30-35% fat
Why this works:
- Higher protein has minimal impact on insulin, promotes satiety, and preserves muscle.
- Lower carbs reduces the glucose load, requiring less insulin.
- Moderate healthy fats slow digestion and support satiety without spiking insulin.
In grams (for 1,800 calories):
- Protein: 160-180g (35-40%)
- Carbs: 112-157g (25-35%)
- Fat: 60-70g (30-35%)
This moderate-carb approach is sustainable and effective for most people with mild to moderate insulin resistance.
Adjusting Ratios by Severity
Your ideal carb intake depends on how insulin resistant you are.
| Severity | Carb % | Carb Grams (approx.) | Description |
|---|---|---|---|
| Mild | 30-35% | 125-150g | Early stages, often lifestyle-induced. |
| Moderate | 25-30% | 100-125g | Clear symptoms, pre-diabetic range. |
| Severe | 20-25% | 75-100g | High fasting insulin, significant symptoms. |
| Very Severe | <10% (Keto) | <50g | Often co-occurs with Type 2 Diabetes. |
How to know your severity:
- Fasting Insulin: <5 (optimal), 5-10 (mild IR), 10-20 (moderate IR), >20 (severe IR)
- HbA1c: <5.5% (optimal), 5.5-6.4% (pre-diabetes)
Work with your doctor to interpret your bloodwork. If you don’t have bloodwork, start with a moderate approach (30% carbs) and adjust based on how you feel.
For a deeper dive into very low-carb diets, see our keto macros guide. For a guide on PCOS, a related condition, see our macros for PCOS article.
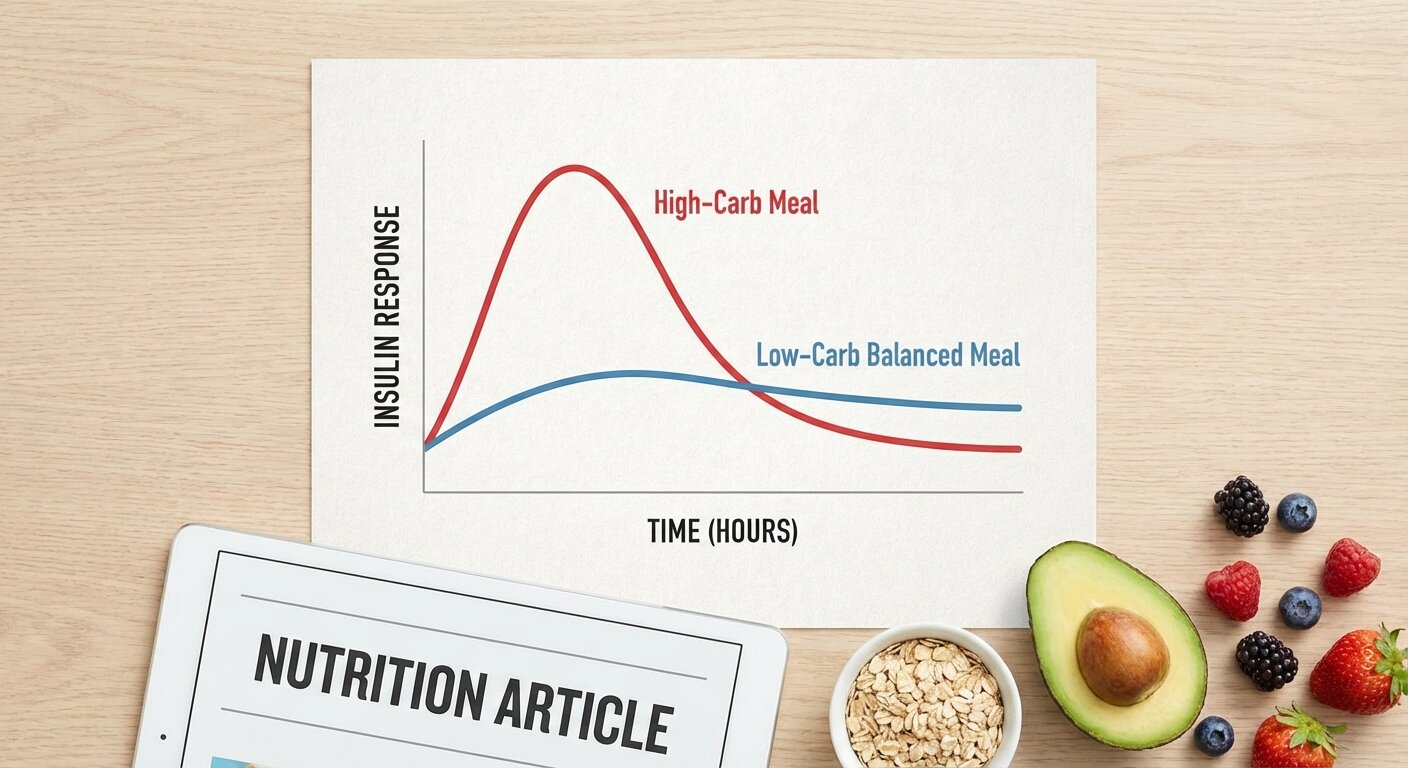
Carbohydrates and Insulin Resistance
Carbohydrates are the most important macro to manage with insulin resistance. Quality matters more than quantity.
The Glycemic Index (GI)
The GI ranks foods based on how quickly they raise blood sugar. With insulin resistance, you want to choose low-GI foods.
Best Carbs (Low GI):
- Non-starchy vegetables: Leafy greens, broccoli, cauliflower, peppers, zucchini (eat freely)
- Legumes: Lentils, chickpeas, black beans
- Whole grains: Quinoa, steel-cut oats, barley, brown rice (in moderation)
- Low-sugar fruits: Berries, apples, pears
- Sweet potatoes and yams
Worst Carbs (High GI - Limit or Avoid):
- Sugar: Soda, candy, baked goods, fruit juice
- Refined grains: White bread, white rice, pasta, crackers, cereal
- Starchy vegetables: White potatoes, corn
- Processed foods: Most packaged snacks
Fiber is Non-Negotiable
Fiber slows down the absorption of sugar, preventing blood sugar spikes.
Target: 30-50g of fiber per day.
High-fiber superstars:
- Chia seeds: 10g per 2 tbsp
- Avocado: 10g per medium avocado
- Lentils: 15g per cup
- Berries: 8g per cup
- Broccoli: 5g per cup
Carb Timing Strategies
1. Pair carbs with protein and fat.
- Never eat a “naked carb” (e.g., an apple by itself).
- Pairing slows digestion and blunts the insulin response.
- Good: Apple with peanut butter. Rice with chicken and avocado.
2. Eat carbs post-workout.
- Exercise temporarily increases insulin sensitivity, so your muscles are primed to absorb glucose.
3. “Bookend” your day with protein and fat.
- A breakfast high in protein and fat (e.g., eggs and avocado) sets you up for stable blood sugar all day.
- A carb-heavy breakfast (cereal, bagel) starts the blood sugar rollercoaster.
Protein for Improving Insulin Sensitivity
Protein is your secret weapon against insulin resistance.
Why Protein is Crucial
- Minimal insulin response: Protein has a very small effect on blood sugar and insulin.
- High satiety: It keeps you full, reducing cravings for the carbs that cause problems.
- Preserves muscle mass: More muscle means more places for glucose to go, which improves insulin sensitivity.
- High thermic effect: Your body burns more calories digesting protein.
How Much Protein?
Target: 1.0-1.2g per pound of ideal bodyweight.
This is higher than the standard recommendation, but research shows higher-protein diets are superior for managing insulin resistance.
Example (Goal weight of 150 lbs):
- 150g - 180g of protein per day.
Best Protein Sources
- Lean meats: Chicken breast, turkey
- Fish: Especially fatty fish like salmon for its omega-3s
- Eggs
- Greek yogurt (plain, unsweetened)
- Legumes (beans, lentils)
- Tofu and tempeh
- Quality protein powder
Spread your protein intake throughout the day (30-40g per meal) to maximize its benefits.

Healthy Fats for Blood Sugar Control
The right fats can improve insulin sensitivity, while the wrong fats can make it worse.
Why Healthy Fats Help
- Slow digestion: Fat slows down the absorption of carbs, preventing blood sugar spikes.
- Reduce inflammation: Omega-3s are potently anti-inflammatory, and chronic inflammation worsens insulin resistance.
- Improve cell membrane health: Healthy fats make cell membranes more fluid and responsive to insulin.
Best Fats for Insulin Resistance
- Monounsaturated Fats: Olive oil, avocados, almonds, macadamia nuts.
- Omega-3 Fats: Fatty fish (salmon, mackerel, sardines), walnuts, flaxseeds, chia seeds.
- Coconut oil and MCT oil: May improve insulin signaling.
Fats to Limit or Avoid
- Trans Fats: Found in processed foods, margarine. Avoid completely.
- Industrial Seed Oils: Soybean, corn, canola, sunflower oils. These are high in omega-6, which can be pro-inflammatory in excess.
- Excessive Saturated Fat: From processed meats and fatty dairy. Small amounts from quality sources are fine, but excess can worsen insulin resistance.
Weight Loss with Insulin Resistance
Weight loss is one of the most effective ways to reverse insulin resistance. Even losing 5-10% of your body weight can dramatically improve insulin sensitivity.
The Challenge
Insulin resistance makes weight loss harder because high insulin levels promote fat storage and block fat burning.
The Solution: A Macro-Focused Approach
- Modest Calorie Deficit: Aim for 300-500 calories below your TDEE. Aggressive deficits can backfire by increasing stress hormones.
- High Protein: Keep protein at 1.0-1.2g/lb to preserve muscle and manage hunger.
- Lower Carbs: Stick to your calculated carb target (25-35%).
- Prioritize Strength Training: Building muscle is non-negotiable. Muscle is a “glucose sink”—it pulls sugar out of your blood, directly improving insulin sensitivity.
Expect slower fat loss. It’s normal. Focus on consistency and non-scale victories like improved energy and reduced cravings.
For more, see our guide on macros for weight loss.
Sample Meal Plan for Insulin Resistance
Target: 1,800 calories | 160g protein (35%) | 135g carbs (30%) | 70g fat (35%)
Breakfast (8 AM)
- Scrambled Eggs & Avocado: 3 whole eggs scrambled with spinach, 1/2 avocado on the side.
- Macros: ~30g protein, 10g carbs, 25g fat
Lunch (1 PM)
- Large Chicken Salad: 6 oz grilled chicken breast over mixed greens with cucumber, bell peppers, tomatoes, and an olive oil vinaigrette.
- Macros: ~50g protein, 15g carbs, 20g fat
Snack (4 PM)
- Greek Yogurt with Berries & Nuts: 1 cup plain Greek yogurt, 1/2 cup mixed berries, 1/4 cup almonds.
- Macros: ~25g protein, 25g carbs, 15g fat
Post-Workout (6 PM - after exercise)
- Protein Shake: 1 scoop whey protein.
- Apple: 1 medium apple.
- Macros: ~25g protein, 25g carbs, 2g fat
Dinner (7 PM)
- Salmon with Quinoa & Broccoli: 6 oz baked salmon, 1/2 cup cooked quinoa, 1 cup steamed broccoli.
- Macros: ~40g protein, 35g carbs, 15g fat
Lifestyle Factors Beyond Macros
Macros are key, but these factors are also critical for reversing insulin resistance.
1. Exercise
- Strength Training (3-4x/week): The most effective exercise for improving insulin sensitivity. More muscle = better blood sugar control.
- Walking (daily): A 10-15 minute walk after meals can significantly lower post-meal blood sugar.
- HIIT (1-2x/week): High-Intensity Interval Training is also excellent for insulin sensitivity.
2. Sleep
- Aim for 7-9 hours per night.
- Just one night of poor sleep can induce temporary insulin resistance. Chronic poor sleep is a major contributor to the problem.
3. Stress Management
- Chronic stress raises cortisol, a hormone that increases blood sugar and worsens insulin resistance.
- Practice meditation, deep breathing, yoga, or spend time in nature.
4. Intermittent Fasting (Optional)
- Fasting periods give your body a break from producing insulin.
- A 16:8 schedule (eating within an 8-hour window) can be effective.
- This is an advanced strategy; nail your macros first.
Tracking Progress
How do you know if it’s working?
Subjective Measures (Weeks 1-4)
- More stable energy levels (no post-meal crashes)
- Reduced cravings for carbs and sugar
- Less “brain fog”
- Better mood
Objective Measures (Months 2-3)
- Weight loss and reduced waist circumference
- Improved Bloodwork:
- Lower Fasting Insulin: The most direct measure.
- Lower Fasting Glucose:
- Lower HbA1c: Your 3-month average blood sugar.
- Improved Triglyceride/HDL ratio: A strong indicator of insulin resistance.
Work with your doctor to monitor your bloodwork every 3-6 months. Reversing insulin resistance takes time and consistency, but the payoff for your long-term health is immense.
FAQ: Insulin Resistance and Macros
What are the best macros for insulin resistance?
The best macro ratio for insulin resistance is typically 35-40% protein, 25-35% carbs, and 30-35% fat. This higher-protein, lower-carb approach helps manage blood sugar, improve insulin sensitivity, and promote satiety. Individual needs vary based on severity and activity level.
How many carbs should I eat with insulin resistance?
Most people with insulin resistance benefit from a moderate carb intake of 100-150g per day. Those with severe insulin resistance may need to go lower (50-100g). Focus on low-glycemic, high-fiber carbs like sweet potatoes, quinoa, berries, and non-starchy vegetables.
Can I reverse insulin resistance with diet?
Yes, insulin resistance can often be significantly improved or even reversed through diet and lifestyle changes. A macro-balanced diet, regular exercise (especially strength training), weight loss, and improved sleep can restore insulin sensitivity over time.
Should I do keto for insulin resistance?
Keto can be very effective for reversing severe insulin resistance due to its very low carb content. However, it’s not necessary for everyone. A moderate-carb approach is often more sustainable and still highly effective for mild to moderate insulin resistance. Try moderate-carb first.
Why is protein important for insulin resistance?
Protein has a minimal effect on blood sugar and insulin. A high protein intake (1.0-1.2g per pound) improves insulin sensitivity, increases satiety (reducing cravings for carbs), and helps preserve muscle mass, which is crucial for metabolic health.
What foods should I avoid with insulin resistance?
Avoid high-glycemic foods that spike blood sugar and insulin. This includes sugary drinks, candy, white bread, pasta, white rice, and processed snack foods. Also limit excessive saturated fat and processed seed oils, which can worsen insulin resistance.
How long does it take to see improvement in insulin resistance?
You may feel better (more stable energy, fewer cravings) within 1-2 weeks. Measurable improvements in bloodwork (fasting glucose, fasting insulin, HbA1c) typically take 8-12 weeks of consistent diet and lifestyle changes.
What’s the difference between insulin resistance and diabetes?
Insulin resistance is a precursor to type 2 diabetes. In insulin resistance, your body produces extra insulin to keep blood sugar normal. In type 2 diabetes, insulin resistance has progressed to the point where your body can no longer compensate, and blood sugar levels become chronically elevated.
Disclaimer: This content is for informational purposes only. Consult a healthcare provider before making changes to your diet.


